CARDS 2 TO 7 OF GOLD
ALZHEIMER´S DISEASE
Cards 2 to 7 of gold: Alzheimer´s disease
Alzheimer destroys our neuronal treasure and the richness of its connections, obscuring memories, limiting cognitive abilities and hindering daily life. The suit of gold symbolizes both the million-dollar investment that research into this disease requires, and the brilliance of science that will end up providing effective treatments to combat it. Brain health is essential to maintain our personal autonomy, preserve memory and enjoy life, but it is threatened by a series of neurodegenerative diseases capable of affecting both our central nervous system (brain – cerebrum, cerebellum, medulla oblongata – and spinal cord) and the peripheral nervous system (ganglia and nerves). Very diverse and complex, all of them are accompanied by a more or less progressive process of chronic neuroinflammation, which ultimately leads to neuronal degeneration and death.

The most common neurodegenerative disease is Alzheimer’s. It is also the main cause of dementia in the world (it causes two thirds of cases).
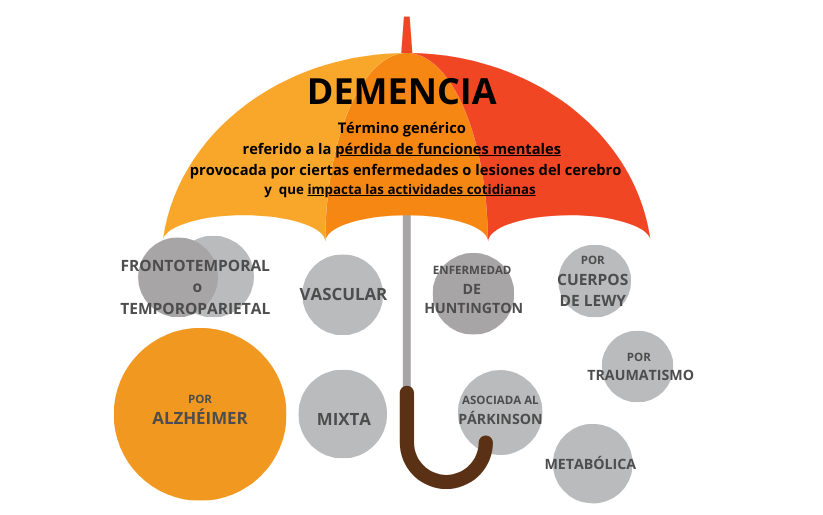
Dementia and Alzheimer’s disease are terms that are often confused. “Dementia” is a generic word that refers to a loss of cognitive abilities that is sufficiently pronounced to interfere with the daily life of the person who suffers from it. It is the manifestation of a set of signs and symptoms produced by some type of brain alteration. Depending on the cause and the brain areas affected, the symptoms and evolution will be different [1]. Currently, dementia of all types affects around 46 million patients worldwide, 8 million in Europe and around 800,000 people in Spain. Every year 4.6 million new cases are diagnosed worldwide [9], but due to the increase in the population and its life expectancy, this number could triple in 2050 to reach 152 million [2]. Today, 60% of people with dementia live in low- or middle-income countries, but in 2050 this percentage will rise to 71%.
It was Emil Kraepelin (1856-1926), pioneer of modern scientific neuropsychiatry in Germany who, in 1910, called “Alzheimer’s disease” the set of symptoms that his disciple Alois Alzheimer (1864-1915) had described for the first time in 1906, associated with the anomalies he observed in the brain of a 55-year-old patient, Auguste Deter. In the Cajal Legacy, histological preparations by Santiago Ramón y Cajal from 1920-1925 are preserved, labeled “Alzheimer’s disease or dementia” [4].
In the autopsy of Auguste Deter’s brain, Alois Alzheimer observed that the cerebral cortex was thinner than normal and that between the neurons there were accumulations in the form of plaques – which he called “amyloids” – because they were stained like starch although in reality they are made of protein nature—and within the neurons themselves there were accumulations of apparently fibrous material—later called “neurofibrillar tangles” or tangles, in English. The presence of these anomalies and accumulations interrupt neuronal functioning and are responsible, over time, for neuronal death [5][6][7].
Alzheimer’s Disease is usually diagnosed in people over 65 years of age, but more and more cases of early onset are emerging. However, the first brain damage may have started up to 15 or 20 years before the appearance of the first symptoms, during a preclinical phase, which is followed by others with mild to moderate symptoms before reaching the severe phase in which it is already established. has produced significant neuronal loss and a consequent reduction in brain volume.
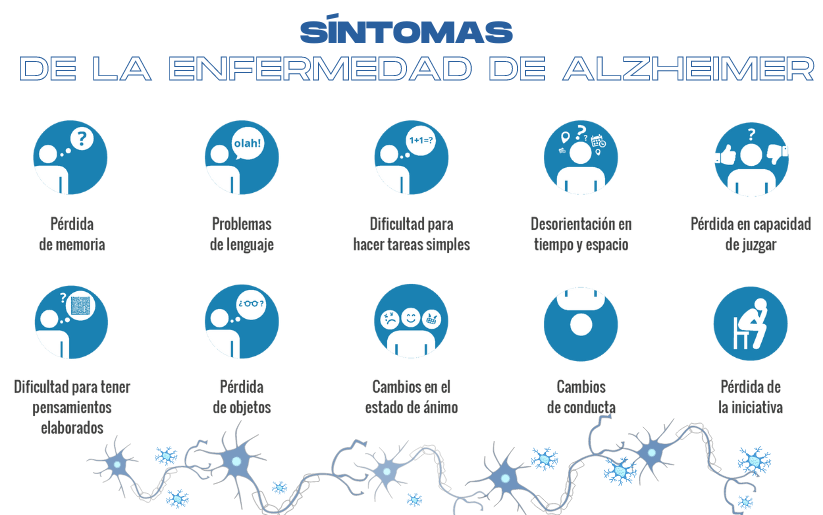
It is a progressive and irreversible disease, characterized by the slow onset of symptoms but whose progressive cognitive deterioration ends up causing dementia. Significant cognitive impairment is characterized by memory loss, language disturbances, loss of sense of direction, and difficulty planning tasks or solving problems. All of this is usually accompanied by changes in character and behavior. Over time, the Alzheimer’s patient loses autonomy and, in the most advanced stages, will need almost permanent help and care.
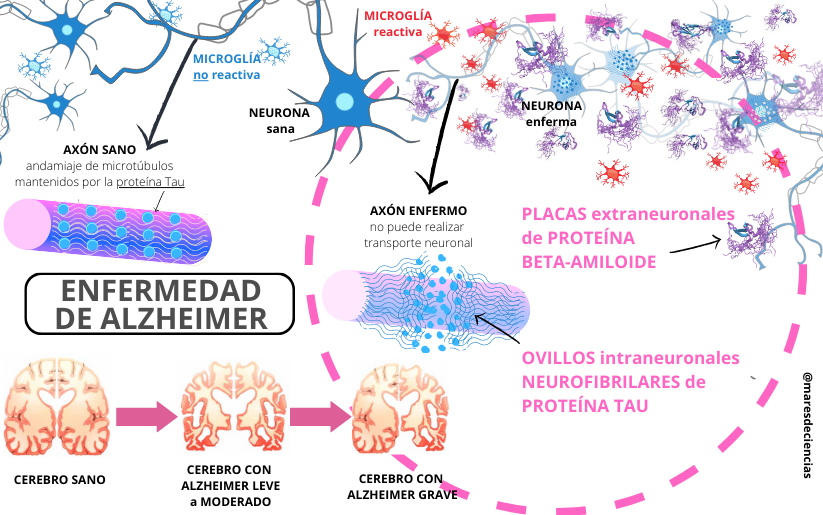
The exact causes of Alzheimer’s disease are unknown, but most scientists agree on the role that two protein substances play in the Alzheimer’s brain, although it is still unknown exactly how they relate to each other. The truth is that Alzheimer’s disease affects both the communication between nerve cells and the cells themselves. In a very simplified way, we know that:
- Amyloid peptides (Aβ) form plaques and accumulate in brain tissue, initially in regions related to memory (the hippocampus) and higher cognitive functions (the cerebral cortex). These accumulations may contain degenerated neuron endings and be surrounded by reactive glial cells. It appears that the accumulation of the Aβ peptide activates microglia, which concentrate around these plaques, but do not eliminate them.When activated, microglia cause the release of pro-inflammatory mediators and glutamate in the area, which ends up killing the neurons. It also appears that phagocytosis, inflammatory cascades, and synaptic pruning are altered, which can become uncontrolled and unduly destroy synapses and neurons.
- The tau protein, which under normal conditions contributes to stabilizing long axons and intervenes in the neuronal transport system (of nutrients, neurotransmitters…) made up of microtubules, also reaches abnormal levels in Alzheimer’s patients and concentrates forming neurofibrillary tangles. that block and destroy this transport system in the axons.Although it is not known what causes the abnormal increase in amyloid peptides, it appears that their accumulation is what causes the increase in tau protein. The disease progresses producing neuroinflammation and atrophy due to the destruction of nerve cells, which causes a shrinkage of the cerebral cortex, the enlargement of the ventricles and the reduction of the hippocampus. In parallel with the decrease in brain volume, glucose metabolism also begins to alter, even before the first symptoms appear [2].
In most cases, Alzheimer’s disease is not hereditary (“sporadic” variant), but there are hereditary risk factors that increase the probability of suffering from it, although they are neither sufficient nor necessary to suffer from it [8]. However, in 1% of patients, the causes can be attributed exclusively to a genetic or hereditary factor (“familial” variant). It seems that in these cases there is a mutation of three genes and the more aggressive disease usually appears before the age of 60 or 65, with a probability of developing the disease for the descendants of 50% [9].
According to Alireza Atri, head scientist at the Alzheimer’s Prevention Initiative, the “toxic chemical” in amyloid is likely to originate from metabolic factors that affect everyone as they age. For example, our ability to metabolize cholesterol and glucose, as well as inflammation, oxidative stress and “malfunctioning of the brain’s waste collection system.” In his opinion, all these elements possibly help to increase the accumulation of amyloid, which in turn causes damage to the synapses and causes the aggregation of the protein tau, the real culprit of the destruction of axons [2].
Despite being a very well described disease with more than 100 years of history, research into Alzheimer’s disease is one of the greatest global challenges facing the scientific and medical community. Unfortunately, the resources allocated to researching its causes and clarifying how it works are much less than those dedicated to other diseases, such as cancer or AIDS. The 2018 World Alzheimer Report [2] points out that, for every 12 studies on cancer, there is only one focused on neurocognitive disorders in general, and not necessarily on Alzheimer’s disease. It is therefore not surprising that it is still a disease that has no cure, although it is urgent to find a solution for the increasingly numerous patients.
To raise awareness among the population about all aspects of Alzheimer’s, the World Health Organization (WHO) declared September 21 as World Alzheimer’s Day in 1994 and since 2011 has dedicated the entire month of September to fighting against ignorance of this disease. neurodegenerative.
Paola Barbarino, CEO of Alzheimer Disease International, proposes that states allocate 1% of the societal costs of dementia to fund research in basic science, improvements in care, prevention and risk reduction, drug development, and public health [ 2]. Without considerable investment in these areas of dementia research, we will not be able to elucidate the mechanisms underlying Alzheimer’s disease, its primary cause.
Since 1998, 100 medications have been tested, of which only four have received authorization and serve to control symptoms. However, it has not yet been possible to design an effective medication to stop the progression of Alzheimer’s or to reverse the cognitive deterioration it causes [1][2][3]. In addition to conventional pharmacological treatment, Alzheimer’s patients require non-pharmacological treatment, focused on improving their quality of life and slowing down the progress of the disease for a time thanks to a range of combined therapies for cognitive and social stimulation.
The lines of research seek a double objective: to identify early neurological changes to control the disease from its beginning thanks to an early diagnosis and to design treatments that control the formation of accumulations of amyloid peptides and the dysfunction of the tau protein. Achieving this double objective is very complex and expensive, both for the industry and for researchers, patients and caregivers. For this reason, it is necessary to launch interdisciplinary research programs, with the participation of public and private organizations, such as the one launched on a European scale in 2015: the European Prevention of Alzheimer’s Disease, (EPAD). It is about designing drugs to address the loss of “wiring” between neurons that causes memory loss in patients, but it must also focus on preventing the death of the neurons themselves.
On a national scale, the Cajal Institute contributes to the research effort through its cutting-edge research program dedicated to brain disorders, with 17 teams of scientists focused on the study of diseases such as Alzheimer’s, epilepsy, Parkinson’s or multiple sclerosis.
The good news is that a healthy lifestyle is a way within our reach to reduce the risk of suffering from Alzheimer’s disease. Go ahead and take care of your synapses!

Have you been curious and want to know more?
ALZHEIMER’S ASSOCIATIONS AND FOUNDATIONS
Alzheimer Foundation Spain: http://www.alzfae.org/alzheimer
Spanish Alzheimer’s Confederation: https://www.ceafa.es/es
Fundaciò ACE, Alzheimer Center Barcelona: https://www.fundacioace.com/es
Pasqual Maragall Foundation
web:https://fpmaragall.org/alzheimer-enfermedad/enfermedad-alzheimer/
blog: https://blog.fpmaragall.org/
Alzheimer Europe, the European organization that brings together 37 associations from 33 countries: https://www.alzheimer-europe.org/
EPAD (European Prevention of Alzheimer’s Disease) is a joint research project of European public and private entities https://ep-ad.org/. Presentation video: https://www.youtube.com/watch?v=Ec5bei45ko4&t=98s&ab_channel=IMIEPAD
Alzheimer’s Disease International is the international federation of Alzheimer’s associations in the world: https://www.caeme.org.ar/alzheimer-la-historia-de-una-enfermedad-que-desafia-a-la-ciencia/
Alzheimer’s Association, in the USA https://www.alz.org/acerca-de-nosotros
SOURCES CITED AND NOTES
[1] What are the types and causes of dementia? In «Let’s talk about Alzheimer’s – The blog of the Pasqual Maragall Foundation» (May 2021) https://blog.fpmaragall.org/tipos-y-causas-de-demencias?hsLang=es
[2] World Alzheimer Report 2018: Cutting-edge dementia research: New frontiers. Published by Alzheimer’s Disease International (ADI), London, September 2018. https://www.alzint.org/u/worldalzheimerreport2018-spanish.pdf A glossary of terms related to Alzheimer’s Disease is included in this report.
[3] The Alzheimer’s vaccine: what’s true? In «Let’s talk about Alzheimer’s – The blog of the Pasqual Maragall Foundation» https://blog.fpmaragall.org/vacuna-alzheimer?hsLang=es
[4] Who is Alois Alzheimer. Alzheimer’s Foundation Spain (November 2015) http://www.alzfae.org/fundacion/164/alois-alzheimer
[5] Alzheimer’s, the story of a disease that defies science. Argentine Chamber of Medicinal Specialties (September 2019) https://www.caeme.org.ar/alzheimer-la-historia-de-una-enfermedad-que-desafia-a-la-ciencia/
[6] Tagarelli A, Piro A, Tagarelli G, Lagonia P, Quattrone A. (2006). Alois Alzheimer: a hundred years after the discovery of the eponymous disorder. Int J Biomed Sci. 2006; 2(2):196-204. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3614590/pdf/IJBS-2-196.pdf
[7] History of Alzheimer’s. Chronology of the disease and its research. In «Let’s talk about Alzheimer’s – The blog of the Pasqual Maragall Foundation» (June 2019) https://blog.fpmaragall.org/historia-del-alzheimer.
[8] Discover with the UMH: is Alzheimer’s hereditary?, by Javier Sáez. UMH Tv https://www.youtube.com/watch?v=O7SN4oXCQsM&t=1s
[9] Keys to Alzheimer’s disease. Downloadable document from the Pasqual Maragall Foundation, 15 pp. Extracted from «Let’s talk about Alzheimer’s – The blog of the Pasqual Maragall Foundation» https://blog.fpmaragall.org/
OTHER LINKS TO SOURCES OF INTEREST
“Alzheimer”, correct spelling. FUNDÉU RAE https://www.fundeu.es/recomendacion/alzheimer-escritura-correcta-1079/
10 myths about Alzheimer’s disease https://fpmaragall.org/noticias/rompemos-mitos-acerca-del-alzheimer-con-motivo-de-la-brain-awareness-week/
How to prevent AD from adolescence http://www.alzfae.org/actualidad/actualidad-cientifica/1134/como-prevenir-la-ea- desde-la-adolescencia.
Article cited: Chapman BP, Huang A, Peters K, et al. Association Between High School Personality Phenotype and Dementia 54 Years Later in Results From a National US Sample. JAMA Psychiatry. 2020 Feb;77(2):148-154. https://jamanetwork.com/journals/jamapsychiatry/fullarticle/2752387
Alzheimer’s disease https://infotiti.com/enfermedad-de-alzheimer/
YouTube Channel Cerebrotes, by Clara García.
Where are memories stored?: Synapses and long-term potentiation (December 2021) https://www.youtube.com/watch?v=vTqWh2yYEbk&ab_channel=Cerebrotes
Synapsis EMP YouTube Channel.
What is Alzheimer’s? (April 2016) https://www.youtube.com/watch?v=WRc1cXJUKoM&ab_channel=SinapsisEMP
Neurodegenerative diseases and dementias https://www.youtube.com/watch?v=XJqT8QRTbF0&ab_channel=SinapsisEMP
World Alzheimer Report 2019: Attitudes towards dementia. Published by Alzheimer’s Disease International (ADI), London, September 2019. https://www.alzint.org/u/WorldAlzheimerReport2019-Spanish-Summary.pdf
Dementia. World Health Organization Press Center, September 21, 2020 https://www.who.int/news-room/fact-sheets/detail/dementia
2021 Alzheimer’s disease facts and figures. Alzheimers Dement. 2021 Mar;17(3):327-406. https://alz-journals.onlinelibrary.wiley.com/doi/epdf/10.1002/alz.12328
KISA, Adnan et al. (2022). Estimation of the global prevalence of dementia in 2019 and predicted prevalence in 2050: an analysis for the Global Burden of Disease Study 2019. The Lancet Public Health, Vol. 7, February 2022: Lancet Public Health 2022; 7: e105–25 Published Online January 6, 2022 https://doi.org/10.1016/ S2468-2667(21)00249
“I am with you”, music and lyrics from La Oreja de Van Gogh about Alzheimer’s disease https://www.letras.com/la-oreja-de-van-gogh-musicas/estoy-contigo/
