CARDS FROM 2 TO 7 OF SWORDS
MICROGLIA IN NEURODEGENERATIVE DISEASES
Two to Seven of Swords: MICROGLIA IN NEURODEGENERATIVE DISEASES
Microglia protect the central nervous system and guard its proper functioning, but when the defensive neuroinflammation it triggers in response to aggression becomes uncontrolled, questions accumulate to which neuroscience seeks answers to address the disorders and diseases it causes.

We know that diseases of the nervous system are very complex conditions that force researchers to deploy their neuroscientific arsenal to answer the questions of why, how and when they occur. Clarifying their causes will put us on the path to finding treatments that, in the absence of curing them, at least slow their progression or alleviate the symptoms of those who suffer from them.
In recent years, it has been discovered that microglia play a crucial role in pathologies of the nervous system, regardless of the cause or the affected region. Natalia Yanguas Casás, from the Puerta de Hierro-Segovia de Arana Research Institute, is an expert in these cells and explains to us in this entry what role they play in different neurological diseases.
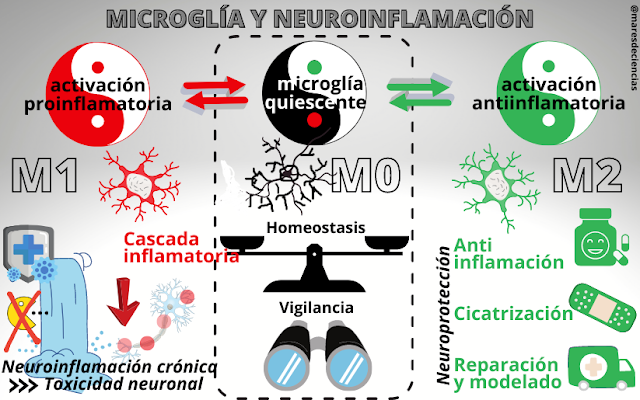
As we saw in the Ace of Swords card in our neurodeck, microglia are the resident immune cell of our nervous system. This means that it is the first line of defense against alterations or possible attacks. How does it perform these functions? Well, first detect the alteration or aggression. It then releases pro-inflammatory substances to activate surrounding cells and recruit others that are further away to eliminate it, in a process called neuroinflammation [1]. Once the problem is under control, the microglial cells phagocytize the cell remains (or debris) that remain in the area and release anti-inflammatory substances so that everything returns to the state of balance (homeostasis) prior to the disturbance, and they can return to their “vigilant” state.
Given the importance of their functions, it is easy to understand that the malfunction of microglia cells is related to the pathogenesis of multiple neurodegenerative diseases. In fact, as we age, microglia become senescent and are not able to resolve the alterations that occur in nervous tissue with the same efficiency as when the organism was younger. Therefore, the incidence of neurodegenerative diseases increases with age [2].
Despite their diversity and complexity, today we know that all diseases of the nervous system are accompanied by a more or less progressive process of chronic neuroinflammation that ends up causing neuronal degeneration and death. However, it is important to know that neuroinflammation is a physiological response generated by microglia cells in order to eliminate disturbances from the environment and keep the nervous system functioning optimally. Normally it is a short-term process, but in pathological situations it becomes chronic, because the microglia are not able to resolve the disturbance and continue releasing pro-inflammatory substances into the environment. In addition, it may not be able to phagocytose the remains of dead cells or misfolded proteins, making the environment toxic to the healthy cells around it.
Microglia are not the only cells that contribute to immunological processes within the nervous system, because other cell populations (such as astrocytes) can respond to pathological factors and influence the responses and reactions of other cells. However, here we are going to focus on the role of microglia in the most common neurodegenerative diseases.
When we present the cards from two to seven of wands we talk about multiple sclerosis, an autoimmune disease in which the immune system attacks the protective myelin sheath that covers nerve fibers, causing communication problems between the brain and the rest of the body. Toxic myelin accumulations generate a pro-inflammatory environment around them that recruits microglia to eliminate them. In the initial stages of the disease, microglia are capable of resolving the situation and reverting the situation to normal, which has been related to the alternation between flares and normal situations in so-called relapsing-remitting multiple sclerosis. But as the immune system continues to attack the myelin sheaths, neuroinflammation becomes chronic and, if combined with failures in myelin phagocytosis, the inflammatory feedback that is generated is increasingly difficult to resolve, until the system no longer can cope and the disease progresses.
With the publication of the cards from two to seven of pentacles we saw that the most common neurodegenerative disease and the main cause of dementia is Alzheimer’s. This disease is characterized by the presence of amyloid peptides (Aβ) that form plaques and accumulate in brain tissue, mainly in the cerebral cortex and hippocampus. Microglia intervene because the Aβ peptide causes its activation and causes it to concentrate around these plaques, which it does not eliminate, however. The activation of microglia also releases pro-inflammatory mediators and glutamate in the area, which ends up killing the neurons. Depending on the stage of the disease, it has been seen that microglia can exert beneficial effects (especially in the initial stages), but when their response is deficient, problems are observed in phagocytosis, in inflammatory cascades, and even in their metabolism.
Another disease with a significant incidence is Parkinson’s, which is the paradigm of neurodegenerative movement disorders, although it also produces alterations in cognitive function, depressive symptoms and pain. The main cause is a deficit in dopamine secretion in a brain region called substantia nigra pars compacta, which is produced by degeneration of neurons in that area. In addition, accumulations of a protein called alpha-synuclein (α-Syn) appear in these neurons, generating what are clinically known as Lewy bodies. It has been seen that α-Syn released by neurons activates microglia, which in this disease present alterations in genes related to oxidative stress and inflammation and in degradation proteins in lysosomes, which means that microglia are capable of phagocytosing them. but not to process them. This results in the exacerbated release of pro-inflammatory mediators by microglia. In addition, it has been seen that the synaptic pruning function, which ensures that neuronal connections work well, is also altered in microglia from animal models and patients with Parkinson’s disease.
Ataxia-telangiectasia is also a neurodegenerative disease related to movement. It is a hereditary disease caused by a specific mutation, which causes degeneration of the cerebellum. Animal models of this pathology have shown that the migration of microglia to the cerebellum is much faster than normal during developmental stages, and that there are also phagocytosis deficiencies in this region.
Another type of neurological diseases are prion diseases or transmissible spongiform encephalopathies, which are produced by proteins called prions, such as Creutzfeldt-Jakob disease (CJD). These pathologies usually debut in middle age and evolve very quickly (90% of patients die one year after diagnosis). It has been suggested that microglia play a crucial role in the initiation of pathological changes in this disease. As in other pathologies with altered protein deposits, microglia are located around them, and are activated to phagocytose them and eliminate them from the environment. Neuronal degeneration in this disease is due to a reduction in resistance to attacks by toxic substances and an increase in the release of these and reactive oxygen species by microglia. Furthermore, microglia activated by prions release pro-inflammatory mediators in that region, aggravating neuronal death.
Epilepsy is a disease caused by alterations in the electrical activity of neurons. The causes are very variable, from genetics to trauma or brain hypoxia, but microglia also play an important role in this pathology. One of the physiological functions of microglia is the pruning of aberrant synapses. This means that for neurons to be able to transmit information from one to another in an optimal way, microglia determine which connections are important and which are not, and eliminate the latter to give priority to the former. If synaptic pruning is not done well, alterations appear in the brain connections that contribute to the pathophysiology of this disease.
Huntington’s disease is rare compared to the previous ones. Its cause is genetic, and therefore it is a hereditary disease. In these patients, and in different animal models, it has been observed that microglia are activated and have a pro-inflammatory phenotype, so that their main contribution to this pathology is, again, the chronification of neuroinflammation.
In addition to its role in neurodegenerative diseases, microglia dysfunction appears in other neurological diseases such as autism or Tourette syndrome (due to deficiencies in synaptic pruning or favoring neuroinflammation in certain stages of development), depression ( due to the release of pro-inflammatory and stress mediators), post-traumatic stress syndrome (promoting inflammation), strokes or trauma (due to dysfunctions in phagocytic capacity and poor resolution of the inflammatory process in some cases) or brain tumors (promoting the migration of tumor cells and tumor escape mechanisms).
It is clear that microglia play a crucial role in diseases of the nervous system, regardless of their cause(s) or the affected area(s). Therefore, like astrocytes, they are currently a very interesting therapeutic target. If we manage to modulate the responses of the microglia, it will be possible to tell them to do what “we want them to do”: from phagocytosing better to eliminate protein accumulations, to determining their type of activation (pro- or anti-inflammatory) depending on the moment. In this way we could change the development of many of these diseases.
Have you been curious and want to know more?
SOURCES CITED AND NOTES
[1] MARTÍNEZ-TAPIA, R. J., F. ESTRADA-ROJO, A. A. HERNÁNDEZ-CHÁVEZ, A. BARAJAS-MARTÍNEZ, S. ISLAS ESCOTO, L. NAVARRO and A. CHAVARRÍA (2018). Neuroinflammation: the Ying-Yang of neuroimmunology. Journal of the Faculty of Medicine (Mexico), 61(5): pp. 44-53 http://www.scielo.org.mx/scielo.php?script=sci_arttext&pid=S0026-17422018000500044&lng=es&tlng=es
[2] If you want to know more about some degenerative diseases, see the entry for cards 2 to 7 of Cups).
OTHER INTERESTING LINKS
PÉREZ CAPOTE, Kamil (2006). Response of glial cells to neuronal damage in vitro. Introduction (55 pp). Doctoral Thesis. University of Barcelona. https://digital.csic.es/bitstream/10261/91949/4/1_INTRODUCCION.pdf
KWON Hyuk-Sung and Seong-Ho KOH (2020). Neuroinflammation in neurodegenerative disorders: the roles of microglia and astrocytes. Translational Neurodegeneration (2020) 9:42 https://translationalneurodegeneration.biomedcentral.com/articles/10.1186/s40035-020-00221-2
Infographic on neurodegeneration (in English)
